Make Every Day Count
Helpful information for family caregivers
September/October 2022
Has your parent remarried? Should a health crisis occur, you will likely be sharing the care with your parent’s spouse. Learn what you can do to increase the chances of a positive partnership. It’s not just your loved one who will benefit. In our middle article we talk about one of the easiest ways to prevent a fall: Working with the doctor or pharmacist to cull out or reduce prescriptions known to cause dizziness, blurry vision, or muscle weakness. Last, we look at the staff you will meet if your loved one needs to stay in a skilled nursing facility. Understanding the roster will help you get the care you want your relative to have.
Caring with a stepparent
 Has your parent remarried? If so, you may be sharing the caregiving with a person you don’t know very well. Biological families often encounter tensions when it comes to eldercare. Add a stepparent and the challenges can grow exponentially.
Has your parent remarried? If so, you may be sharing the caregiving with a person you don’t know very well. Biological families often encounter tensions when it comes to eldercare. Add a stepparent and the challenges can grow exponentially.
At its best. A stepparent can be a wonderful partner in care. Their daily companionship and support may be very meaningful to your parent. Plus, it’s easier to accept assistance with intimate tasks from a partner than from a child. Ask them how you might be of help. It may be running errands, talking with the doctor, communicating with other siblings, paying for extra help, or giving your stepparent a break now and then. Celebrate victories with them: A successful surgery, a clear cancer report. And don’t forget to thank your stepparent regularly for all they do.
Sometimes it’s complicated. Many adult children believe that their stepparent is standing between them and their mom/dad. Or them and the doctor. Perhaps. Or it may be that the spouse is simply overwhelmed or distressed. They could be waiting until there’s a diagnosis and plan in place to tell you there’s a problem. Remember, a health crisis is a crisis in their marriage. They may not have discussed beforehand how they would handle medical emergencies or serious illness. Until you know otherwise, assume everyone is doing the best they can.
Respect roles. Become allies. If your parent named you as health care decision maker in their advance directive, plan ahead with your parent and stepparent about when you would like to be informed of a problem and how the three of you can work together. If at some point you have a “better” treatment path to suggest, consider: Will it require more work for one or both of them? Can you ease the burden? If not, you may need to bow to what your parent and stepparent feel they can handle. If your stepparent is the health care power of attorney, ask for permission before trying to speak with the doctor. Ideally, manage your concerns in a way that avoids creating strife in the marriage, as that truly doesn’t benefit your parent. Respect the decisions they have made and find common cause to cooperate with your stepparent to make your mutual loved one’s recovery or final days as positive and stress free as possible.
Return to topCould medicines be the culprit?
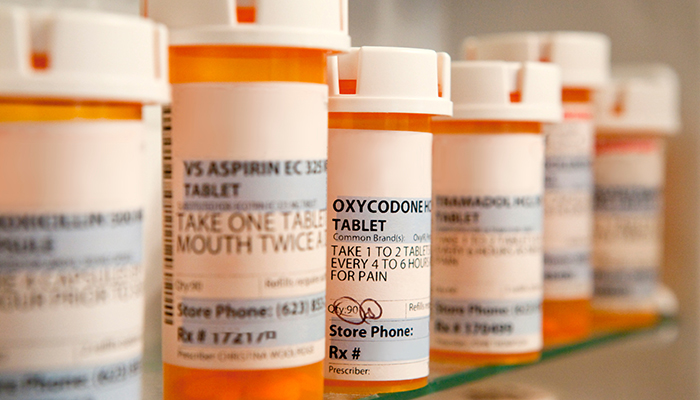 If your loved one has balance problems, the culprit may be in the medicine. Many common medicines have side effects that can impair balance and lead to a fall. Over 40% of persons age 65 and older take five medications or more. This increases the chance that at least one of the drugs has side effects of dizziness, blurry vision, drowsiness, or muscle weakness. Or affects balance sensors in the inner ear. More medications also create the potential for a drug-to-drug interaction that leads to a fall.
If your loved one has balance problems, the culprit may be in the medicine. Many common medicines have side effects that can impair balance and lead to a fall. Over 40% of persons age 65 and older take five medications or more. This increases the chance that at least one of the drugs has side effects of dizziness, blurry vision, drowsiness, or muscle weakness. Or affects balance sensors in the inner ear. More medications also create the potential for a drug-to-drug interaction that leads to a fall.
Medicines known to increase the risk of falls include
- allergy drugs (antihistamines)
- antidepressants and antianxiety drugs
- blood pressure and heart drugs
- diabetes drugs
- pain drugs
- sleep drugs
If your loved one has fallen or seems unstable on their feet, ask the doctor or a pharmacist for a medication review. They may suggest some of the following strategies:
- Reduce the number of drugs. Sometimes a specialist orders a drug without knowing that another doctor has ordered a similar drug.
- Lower the dose. Ask the doctor or pharmacist for their recommendation.
- Change medication. There may be another drug that will accomplish the same treatment but does not have side effects that could cause a fall.
- Altering the schedule. By changing when drugs are taken, you may be able to reduce the side effects or risk.
- Nonpharmaceutical approaches. Relaxation techniques and good sleep hygiene habits might relieve the need for sleep medicine. More exercise and weight reduction could lower the need for insulin.
Do NOT make these decisions on your own. It is important to have the doctor or a pharmacist review all medications and over-the-counter drugs, because they will know which ones to target and the safest way to make changes.
Return to topWho is who in skilled nursing facilities?
 If your loved one is discharged from the hospital to a skilled nursing facility (SNF), their care will be in the hands of a team of specialists. It’s a good idea to understand the players’ roles so you know whom to call upon for what.
If your loved one is discharged from the hospital to a skilled nursing facility (SNF), their care will be in the hands of a team of specialists. It’s a good idea to understand the players’ roles so you know whom to call upon for what.
- Director of nursing. This professional oversees residents’ medical issues. Also, the nursing staff. Their job includes tracking delivery of prescriptions and monitoring each resident’s physical health. They also work with the SNF’s doctor to carry out orders for therapy.
- Social workers. Trained to address social, emotional, and psychological issues, social workers help residents and families adjust to life in the facility. When the time comes for discharge, they also help ease the transition. If there’s something you want done differently with your loved one, you might start a conversation with the social worker.
- Certified nursing assistants (CNAs). The CNAs are the frontline staff. From answering a call button to helping with bathing and dressing, they are often the biggest part of your relative’s daily experience.
- Therapists. Depending on your loved one’s challenges, daily therapy may be required. A physical therapist helps improve walking, range of motion, stamina, and flexibility. A speech therapist helps residents recover language abilities. Or overcome swallowing problems. An occupational therapist uses exercises and assistive devices to regain daily life skills. They teach new strategies for self-care tasks such as feeding, dressing, and bathing.
- Dietitian. Every resident has a food plan. This is based on their personal preferences and any medical restrictions (e.g., low fat, low salt, low sugar).
- Activities director. This professional organizes activities for residents’ social and mental stimulation.
- Housekeeping. Is the bed rail not releasing? Is there a spill to be cleaned? These are responsibilities of the housekeeping staff.

